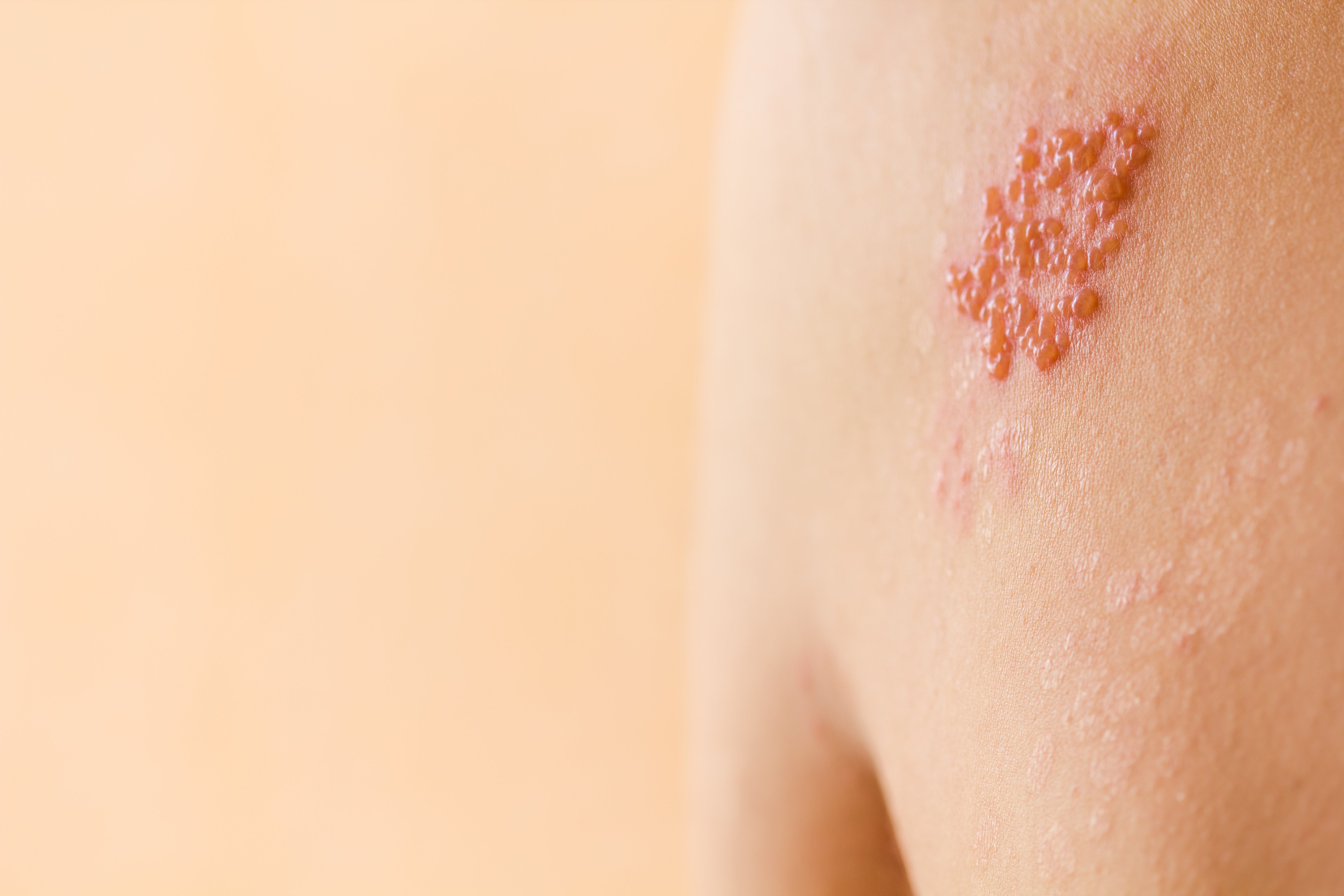
‘Histamine intolerance’ is a condition that results in high histamine levels. It’s caused by a deficiency of an enzyme that breaks histamine down, diamine oxidase (DAO). Anything that increases histamine can contribute to this condition.
Often, a variety of food chemicals can spike inflammation and histamine levels, as was the case in myself.
In addition to my own battle with histamine intolerance, I have had quite a few clients who deal with histamine intolerance. This protocol is dedicated to them. Read on to learn about histamine intolerance, how it affects your health, and what you can do to treat it.
What is Histamine Intolerance?
Causes
Histamine intolerance is a result of too little histamine-degrading enzyme in your gut (DAO), which leads to accumulated histamine and numerous accompanying symptoms that resemble an allergic reaction.
It can come from gut damage, alcohol, drugs/supplements, or a microbial imbalance.
If a lack of DAO is the sole cause of your histamine issues, then all you need to do is take the enzyme.
I suspect, however, that many people who complain of histamine intolerance don’t always have issues with the enzyme in particular. Rather, I believe such people are Th2 dominant and just produce excess histamine after meals.
Another big contributor to histamine intolerance is chronic HPA activation.
For this post, I will discuss all the ways in which you can reduce histamine overall, not only ways to increase the enzyme.
Signs and Symptoms of Histamine Intolerance
The clearest sign of histamine intolerance is a bad reaction after eating fermented foods like sauerkraut.
Reduced DAO levels can lead to the following symptoms [1, 2, 3]:
- Skin problems such as rashes, itch, hives, flushing, eczema, psoriasis, and even acne
- Chronic headaches
- Dysmenorrhea
- Gastrointestinal symptoms
- Nasal mucus
- Asthma attacks
Increased blood histamine levels can trigger a range of unpleasant and even dangerous reactions [4]:
- 1-2 ng/mL: increased stomach acid secretion with flushing, headache, hives (urticaria), and itching skin
- 3-5 ng/mL: increased heart rate
- 7 to 12 ng/mL: bronchospasm (tightened airways)
- 100 ng/mL: heart attack
Thus, large amounts of ingested histamine can cause significant symptoms in otherwise healthy people. For example, the above symptoms may occur following the consumption of spoiled fish, which is high in histamine [5, 6].
Due to the nature of the symptoms caused, the reaction may be incorrectly diagnosed as a food allergy.
Histamine Intolerance Supplements & Treatment Options
Protocol for Histamine Intolerance
If you have histamine intolerance, some potential therapeutic options include:
- Reduce lectin and tannin consumption
- Distress and reduce HPA activation
- Quercetin to stabilize mast cells
- Take probiotics: B infantis, B longum, and L Plantarum to degrade histamine [7, 8, 8]
- Stay away from fermented and cured foods
- Take Allegra in the morning or Benadryl at night to block histamine receptors. Benadryl increases DAO as well [9]
- Take 1,000 mg of vitamin C twice a day [3]
- Vitamin B-6 (Caution: this also increases histidine decarboxylase) [3]
Protocol for Histamine Issues in General
If you have histamine issues in general, then do the following:
- Use Cromolyn as a mast cell stabilizer. It is effective when used right before or during a reaction
- Take 1 capsule of Forskolin as a mast cell stabilizer [10]
- Take 1 capsule twice a day of EGCG to inhibit histidine decarboxylase and stabilize mast cells
- Experiment with other substances below and in the Th2 dominance page
Talk to your doctor before taking any over-the-counter drugs like Allegra or Benadryl.
Low-Histamine Diet
One study found that a diet low in vasoactive amines alleviated chronic headaches in 73% of patients [4].
Another study reported that 27 out of 44 (61%) subjects had a significant improvement in skin reactions on a diet low in dietary amines, additives, and natural salicylate [11].
Subjects with chronic hives or angioedema used less anti-allergy drugs on a histamine-reducing diet [12].
58% of adult patients with irritable bowel syndrome (IBS) considered foods rich in vasoactive amines—such as wine, beer, salami, and cheese—to be a cause of their symptoms [13].
To help combat histamine intolerance and minimize food sensitivities, I came up with the lectin avoidance diet, along with a cookbook.
 Foods to Avoid
Foods to Avoid
The following foods generally have high histamine levels [14, 3]:
- Fermented products: Sauerkraut, kombucha, pickles, fermented soy products, yogurt, buttermilk, kefir, mature cheese
- Alcoholic drinks (not distilled): wine, beer, cider
- Cured, smoked, and fermented meats: Sausage, pepperoni, salami, etc.
- Canned fish products
- Tomato paste
- Spinach and yeast products
According to one study, the average levels of histamine in wine were 3.63 mg/L for French wines, 2.19 mg/L for Italian wines, and 5.02 mg/L for Spanish wines [15].
Biogenic or vasoactive amines are produced by bacteria during fermentation, storage, or decay. They include tyramine, tryptamine, putrescine, cadaverine, spermine, and spermidine, etc., but histamine is most frequently linked to food-related symptoms [4, 4].
Foods likely to contain high levels of these biogenic amines are fermented foods or foodstuff exposed to microbial contamination during storage [14].
The main bacteria responsible for biogenic amine production are lactic acid bacteria (LAB); they break down amino acids into bioactive amines [7, 14].
Citrus fruits are histamine “liberators” and should likewise be avoided [3].
Mast Cell Stabilizers
Mast cell stabilizers reduce histamine by preventing its release from mast cells, or “stabilizing” them.
A relatively safe and effective drug that stabilizes mast cells is called Cromolyn. This drug works via multiple mechanisms in combating allergies. It’s available over the counter in the US.
The following also stabilize mast cells:
- Quercetin [16, 17]
- Fisetin [17]
- Forskolin [10]
- Luteolin [18]
- Apigenin [18]
- Astragalus/Astragalin [17]
- EGCG [19]
- Palmitoylethanolamide
- Methylxanthines
- Reishi [20]
- Chinese skullcap [21]
- Eleuthero [21]
- Kaempferol [17]
- Myricetin [17]
- Rutin [17]
- Theanine [22]
- Tulsi/holy basil [23]
Antihistamines
Antihistamines (H1-receptor antagonists) block histamine receptors and thus silence its effects.
Fexofenadine or Allegra seems like a safe drug that doesn’t cause drowsiness because it doesn’t cross the blood-brain barrier much. First-generation antihistamines (Benadryl) do cross the brain barrier and cause fatigue.
Research on humans taking Allegra at normal dosages shows no significant adverse effects when compared to a placebo.
Benadryl is good to take at night since it induces sleepiness. It’s actually an FDA-approved sleep medication.
Benadryl has other positive effects besides blocking histamine receptors. It decreases anxiety, increases serotonin, increases dopamine, and is useful for the treatment of OCD [24, 25].
Note: Make sure to speak to your doctor before taking any drug or supplement.
Probiotics
Some probiotics degrade histamine and are recommended for histamine-intolerant people; these include:
- B infantis [26]
- B longum [26]
- L Plantarum [14]
People with histamine intolerance generally do better with Bifido probiotics.
Other helpful supplements include pancreatic enzymes and SAM-e [3].
DAO Supplements
Besides taking an enzyme, you can increase DAO production by using the following supplements:
- Vitamin C (500-2,000 mg) [27, 28]
- Vitamin B-6 (caution, this also increases histidine decarboxylase) [3]
Avoid these Supplements
Histamine-producing bacteria:
- L. casei [29]
- L. reuteri[30]
- L. bulgaricus [29]
DAO inhibitors:
- Alcohol [31]
- Curcumin [32]
- Carnosine [33]
- Imidazoles: Found in many plants, especially alkaloids, which include caffeine, nicotine, and theobromine in cocoa [33]
- Cimetidine: An antihistamine [34]
Other:
- Supplements that decrease Th1/Increase Th2
- Quinolone antibiotics may cause histamine release [35]
Factors that Activate Mast Cells & Raise Histamine
Mast Cell Activation, Intolerance & Allergies
Other than histamine, mast cells release:
- Serotonin
- Superoxide (causes brain fog, low T3)
- Heparin (anticoagulant)
- Tryptase
- Thromboxane (clot-forming)
- PGD2 (constricts airways, cause baldness)
- PAF (causes atherosclerosis)
Mast cells are present in most tissues, especially in areas that interact with the outside world: the skin, lungs, digestive tract, mouth, eyelids, and nose.
Their activation plays a central role in asthma, allergic rhinitis, anaphylaxis, eczema, itching (pruritus), hives, pain, and autoimmunity.
 1) Stress
1) Stress
Whenever your stress response is set off, your hypothalamus releases Corticotropin-Releasing Hormone (CRH), which results in cortisol spikes.
Mast cells get activated by CRH, which leads to histamine release; on the other hand, cortisol inhibits histamine secretion in cells [36, 37].
So, we see that stress has opposing effects on histamine. But eventually, you become insensitive to the histamine-reducing effects of cortisol, while CRH stays elevated.
CRH also activates brain mast cells to release inflammatory cytokines such as IL-6 and IL-8. Activation of mast cells by CRH increases brain barrier permeability [38, 38].
Some people produce high levels of CRH and lower levels of cortisol, and this causes a lot of histamine issues.
Through my consults, I’ve realized that a majority of people’s histamine issues are most impacted by chronic stress response activation, i.e., too much HPA activity.
Psychological stress is only one of the dozens of reasons why your stress response is overactive. However, it’s often the most significant factor.
Read the full list of reasons for chronic stress pathway activation and see how many factors apply to you.
Mice who were exposed to acute stress more quickly developed multiple sclerosis, a disease with a leaky brain barrier. When these mice were lacking mast cells or CRH, the effects disappeared [38].
2) Th2 Dominance
If you’re Th2 dominant, you will likely have issues with histamine.
This is because B-cells produce IgE antibodies, which in turn stimulate mast cells to release histamine.
Therefore, you should think about taking supplements to suppress your Th2 system.
3) Biotoxin Illness/CIRS
People with biotoxin illness generally have issues with histamine-rich foods, such as cured or fermented foods.
The most common biotoxin is mold, which is in all of our homes to one degree or another. Mold is a broad category that includes Aspergillus, Stachybotrys, and other species of yeast.
However, it’s usually not just the mold, but also the algae, bacteria, VOCs, and chemicals from the mold that can be mass activators of inflammation, causing histamine issues as a side effect.
The most common markers of biotoxin illness are elevated C4a and TGF-beta. These inflammatory responses activate mast cells, which cause blood histamine levels to rise [39].
4) Chronic Infections
Sometimes, if people have chronic infections, they can have histamine/mast cell issues. Mast cells get activated by parasites through IgE responses, for example [40].
5) Lectins
Lectins can bind to the lining of the gut wall and make it leakier; undigested lectins can enter the bloodstream [41, 42].
Lectins such as ConA are probably the best-studied food components in triggering mast cells and basophils [43].
IgE antibodies contain sugar molecules that are a target of lectins; their binding can trigger histamine release from mast cells.
Here’s how it works (the Ys are IgE antibodies, the red dots are the sugar molecules, and the purple egg is a lectin):
Lectins from the following foods can increase histamine release:
- White potatoes and unmodified potato starch (STA) [43]
- Tomatoes [43]
- Soy (SBA) [44]
- Gluten-containing grains (WGA) [45, 46, 45]
- Legumes (ConA) [44]
6) Leptin
Leptin receptors are present on mast cells in the skin, lungs, gut, and urogenital tract, suggesting that leptin has some effect on mast cells [47].
In metabolic syndrome patients, there was a positive correlation between leptin levels and the number of fat tissue mast cells, suggesting that leptin may stimulate mast cells [48].
It seems like leptin causes mast cells to be more inflammatory [49].
Leptin correlates with mast cell activation in children with asthma [50].
7) Nerve Growth Factor (NGF)
Nerve Growth Factor (NGF) may activate mast cells and causes the release of histamine, thus contributing to histamine intolerance [51].
A number of autoimmune conditions have high NGF as well as more mast cells. NGF is one mechanism by which stress increases histamine intolerance, inflammation, and autoimmunity [52, 52].
8) Ghrelin
Ghrelin and obestatin induce hunger, anxiety, and mast cell activation [53].
This hormone is another reason why anxiety often goes together with histamine intolerance.
9) Fluoride
Fluoride potentiates mast cells to trigger more easily. People are exposed to more fluoride in the US because water is fluoridated.
10) Bradykinin
Bradykinin is a protein that dilates blood vessels and therefore drops blood pressure; it is used in studies to increase histamine levels [54].
ACE inhibitors (blood pressure-lowering drugs) increase bradykinin. They can also constrict our airways, which makes sense because histamine causes such effects.
Therefore, people with histamine issues would be wise to stay away from ACE-inhibiting drugs, unless absolutely needed.
Supplements that inhibit bradykinin:
- Bromelain [55]
- Aloe [56]
- Grape seed extract and polyphenols [57]
11) Histidine Decarboxylase
Histidine decarboxylase (HDC) is the enzyme that speeds up histamine production from the amino acid histidine. This enzyme is helped by vitamin B6.
It might be a good idea to test for H Pylori; it affects about 52% of the American public and increases HDC [58].
HDC Inhibitors
If you inhibit the enzyme HDC, you decrease the production of histamine. Inhibitors of HDC are:
- Glucocorticoids/cortisol/dexamethasone [59]
- EGCG/catechins – found in green tea
- Naringenin [60]
- Mucuna/L-DOPA (strong) [61]
- NAC (strong; however, NAC increases histamine) [62, 63, 64]
- SAM-e (strong) [61]
- Urocanic acid (strong) [61]
- Carnosine (less strong) [64, 33]
- Valine (weak) [61].
- Oxaloacetate (weak) [61]
12) Low Erythropoietin
In a clinical trial with uremic patients, 8 out of 10 people with pruritus had marked reductions in their pruritus scores during erythropoietin therapy.
Therapy with erythropoietin decreased histamine, and discontinuation of erythropoietin was accompanied by increases in histamine [65].
Read a list of ways to increase EPO.
13) Melanocortin
People with histamine issues are often underweight, have low blood pressure, have increased pain sensitivity, and don’t display fever.
While histamine has a role in these, activation of the melanocortin receptors can cause the same issues (MC4R) [66].
People with chronic stress and/or inflammation have the MC4R receptor activated, which then leads to flushing, weight loss, lower blood pressure, and increased pain [66].
My guess is that both histamine and MC4R cause flushing symptoms.
You can check your genes for MC4R.
14) Sulfation Problems
Some people supposedly have trouble converting sulfur to sulfate (phenol sulfotransferase issue), and they often times develop a high histamine level. Avoiding certain phenolic and high salicylate foods may help the sulfation problem and subsequently lower histamine.
MSM or Epsom salts also supply sulfur to the system and may be helpful, though some people cannot convert the sulfur in MSM to the needed sulfate form. Taking MSM or Epsom salts may alleviate a histamine reaction. You can also try glucosamine and chondroitin sulfate.
15) Genetic Factors
If you’re not interested in genetics and haven’t done a DNA test yet, skip this part!
If you have one of the gene variations that results in lower DAO, you are more likely to have a surplus of histamine and histamine intolerance. Check out this post for more info.
SelfDecode is the best and most powerful genetic application, which helps you interpret your genes. You need to sign up and upload your genetics to see what versions of these genes you have.
Head over to these posts on our personalized genetics blog to find out if you are genetically vulnerable to high histamine:
- How to Combat Histamine Intolerance Through Genetics (DAO Gene)
- Are You Genetically Vulnerable to High Brain Histamine, Migraines, or ADHD? (HNMT Gene)
SelfDecode is a sister company of SelfHacked. The proceeds from your purchase of this product are reinvested into our research and development, in order to serve you better. Thank you for your support.
SNPs in the HDC gene:
Some HDC gene variants increase the risk of developing allergic rhinitis [67].
| Gene name | SNP/variants | Effects of snps/variants |
|---|---|---|
| HDC | rs16963486 | Decreases HDC activity, increases histamine levels |
SNPs in the HNMT gene:
A variant of HNMT increases the risk of developing atopic dermatitis in children twofold, while another variant is associated with chronic urticaria [67].
The HNMT gene, also known as C939T, regulates histamine. “AA” will increase histamine; if you have AA don’t despair, as ~56% of the population has this genotype.
“AA” for this gene indicates an increase in ADHD behavior for children exposed to certain food additives: Sunset yellow, carmoisine, tartrazine, ponceau 4R, quinoline yellow, Allura red AC, and sodium benzoate.
Scientists think that “AA” increases histamine levels, which is responsible for ADHD behavior [68].
Taking SAM-e should negate this gene, theoretically.
SNPs in the Diamine Oxidase gene (AOC1):
rs10156191 and rs1049742 (AOC1): Each T allele means you have reduced DAO activity and thus higher histamine [69, 69].
SNPs in the H4R gene:
Variants of the H4R gene are associated with an increased risk of atopic dermatitis, and infection-induced asthma [67, 70].
The number of H4R copies correlates to the incidence of arthritis, proteinuria, and antinuclear antibody abnormalities in systemic lupus erythematosus (SLE) [70].
SNPs in the H1R gene:
A variant in H1R has been associated with Parkinson’s disease [67].
SNPs in the MS4A2 gene:
The MS4A2 (Membrane-spanning 4-domains A2) gene codes for a subunit of the IgE-receptor protein. The IgE-receptor protein is found on the surface of mast cells and plays an important function in allergen response [71].
Mutations in this gene are associated with asthma and fibromyalgia, among other conditions [72, 73].
SNPs in the GABRB3 gene:
The GABRB3 gene encodes a protein that serves as the receptor for gamma-aminobutyric acid, a major inhibitory neurotransmitter of the nervous system. It is associated with epilepsy and autism [74].
Histamine Intolerance Test
Diagnosis
You can do a histamine test to check for elevated blood levels. You can also check your tryptase levels, which are markers for mast cell activation.
The diagnosis of sensitivity to vasoactive amines is usually made through history and dietary exclusion; however, some studies have suggested that the measurement of diamine oxidase (DAO) levels may be helpful.
One study found a DAO level <3 kU/mL was associated with reported symptoms to high histamine foods, whereas histamine intolerance was unlikely at a level of >10 kU/mL [75].
Patients with chronic hives/urticaria and GI symptoms have reduced DAO activity [76, 77].
The size of the wheel used in the “histamine 50-skin-prick test” can be a useful diagnostic indicator: in one study, 82% of subjects with histamine intolerance maintained a wheal size greater than 3 mm, compared with 18% of controls [78].
I suggest just taking the DAO enzyme and see how you feel.
Takeaway
The most common cause of histamine intolerance is a deficiency in DAO—an enzyme that breaks down histamine—due to gut damage or a microbial imbalance. It manifests with skin reactions and digestive symptoms after consuming histamine-rich foods and drinks. Foods high in histamine and other vasoactive amines include fermented products such as sauerkraut, dairy, processed meat, beer, wine, and canned fish. If you have histamine intolerance, stay away from these items and try The Lectin Avoidance Diet. Mast cells liberate histamine in response to allergens and other triggers such as stress, Th2 dominance, parasitic infections, mold, lectins, fluoride, and certain hormones. Antihistamines (Allegra, Benadryl) and mast cell stabilizers (Cromolyn) are the main histamine-lowering drugs. Helpful supplements include Bifido probiotics, vitamins C and B6, pancreatic enzymes, SAM-e, quercetin, and EGCG.


