This post is part of a series that’s deconstructing the immune system in various ways. I spoke about Th1/Th2 dominance and wrote multiple posts on how to reduce it. I also spoke about TNF, which is one of several really common cytokines that can destroy our health and performance.
Interleukin-1 is another one of those performance-killing cytokines that can cause us ill health.
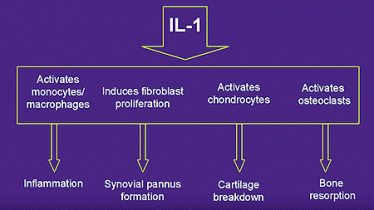
What is Interleukin-1 (IL-1)?
Twenty-five years ago, immunologists and neuroscientists had little science mutual interest. This is no longer the case. Neuroscientists now know that cytokines like IL-1 interact with neurons of the hypothalamus in many ways (by suppressing orexin, etc) [1].
Macrophages and a bunch of immune cells produce and release IL-1b and TNF [2]. Both are usually elevated together because each increases the other [3, 4], so it’s hard to tease out what plays a more significant role. TNF makes IL-1b “active” [4] and IL-1b also increases TNF inflammation [3], making the two synergistically harmful.
IL-1 has two main forms: IL-1b and IL-1alpha. IL-1b seems to be the most significant in relation to disease and there’s more research on it because it possesses a strong pro-inflammatory effect.
If IL-1 is at significantly high levels, it causes fever, increased pain sensitivity, vasodilation, and hypotension [5]. I had the latter 3, but not so much of fever. This cytokine has a natural antagonist, which counteracts its effect – IL-1Ra (IL-1 receptor antagonist).
IL-1 can be elevated in either Th1 or Th2 dominance [6].
Fibrinogen (causes clotting) and CRP are increased by IL-1b [7], but these aren’t usually elevated unless your cytokines are acutely increased.
IL-1b is necessary for replicating Th17 immune cells [8]. It also increases nitric oxide and PGE2 [9].
IL-1b will stimulate your HPA axis and sympathetic nervous system, which both go on to lower other cytokines like TNF [10].
Like everything else, baseline IL-1b production and production in response to stimuli is genetic. The SNP rs16944 is a polymorphism in the interleukin 1, beta gene and different versions of it are associated with higher and lower risks of various diseases.
It’s important to realize that you can have IL-1b elevated locally in areas such as your hypothalamus or gut and it wouldn’t show on blood tests.
IL-1b and Me
I suspect (just a theory) that I had a history of high IL-1b in my hypothalamus and gut, which caused me to get fatigued via suppression of orexin neurons [11] and this would subsequently activate my HPA axis, in order to suppress inflammation.
The result was an HPA axis that went into overdrive even though I had no perceived stress.
One possible contributor is CCK. I’m a high producer of CCK, which stimulates the vagus nerve. Indeed, I have a lot of symptoms of vagus nerve activation (low heart rate, blood pressure, appetite).
Stimulation of the vagus nerve increases IL-1b in the hypothalamus and the hippocampus, which goes on to activate the stress response [12].
However, vagus nerve stimulation also causes low systemic inflammation, which would make sense for me.
The Good
IL-1b is part of the mechanism of inducing sleep and increases non-rem sleep and the time it takes to fall asleep [13, 14]. It works in part by increasing adenosine. Therefore, this is not something you want to inhibit during the night.
In rodents, IL-1b increased the release of oxytocin and vasopressin [15]. Oxytocin is usually ‘good’.
IL-1b increases NGF [16]. NGF, along with NT-3, are somewhat unique in stimulating neurite growth, which can’t be done by NGF, BDNF or NT-4 alone [17]. IL-1b also increases GDNF [18], which again stimulates neurite outgrowth. In addition, it can increase dopamine-promoting neurons by increasing bFGF [19].
So while IL-1b is neurotoxic, it can increase the growth of neurons [18]. My advice is to allow this effect when you are supposed to have it: while you’re asleep. While my mind worked better in some limited ways with inflammation, it’s overall much better now.
IL-1b can also increase the release of dopamine, norepinephrine, and serotonin in the frontal part of the hypothalamus [20]. (don’t know if this is good)
Even a relatively low level of IL-1 decreases aldosterone synthesis in response to ACTH (precursor of cortisol), which increases in response to stress and intense exercise [21]. This can lower blood pressure. IL-1b, however, actually increased aldosterone synthesis by a bit.
I suspect that I used to have low aldosterone, which manifested itself as low blood pressure and exercises headaches/hyponatremia. I believe this was because of the inflammation I was experiencing. Exercise increases ACTH, which normally tells our body to conserve salt by increasing aldosterone. However, if we have inflammation, then aldosterone production will be limited and if we sweat a lot it can cause low levels of salt in the body, causing hyponatremia.
The Bad
I spoke about how trying to increase our motivation or mood by hacks, tricks or by changing our mindset will only increase our neuroticism and delays acceptance of our present reality. However, I support trying to modulate these factors by biological manipulation.
If you have elevated IL-1 then that will affect your mood, cognitive function, levels of wakefulness and motivation and lowering the chronic inflammation is what you need to be focusing on.
IL-1 plays a major role in many diseases and is a cytokine that is a performance killer. It does this in part by inhibiting orexin, which is a central regulator of many bodily functions, but also by many other pathways.
For example, depression can be caused by IL-1 [22, 23], and it may be the cause of your bad moods.
IL-1b decreases the synthesis of estrogen and increases the breakdown of progesterone [24], both of which are anti-anxiety hormones [25, 26]. It can also decrease male hormones (in response to hCG stimulation) [27].
Stress causes depression via an IL-1b mediated mechanism [28].
IL-1 also harms cognitive performance. IL-1b is detrimental to neuronal synapses during activation-induced inflammation and causes neurodegeneration [29]. It can also negatively impact Long-Term Potentiation [30], which is critical for learning and memory. My memory and cognitive function have improved as I lowered this cytokine in myself.
A significant mechanism for these effects is likely decreased Brain-Derived Neurotrophic Factor (BDNF), which is inhibited by IL-1b (at least its end products like CREB) [31].
IL-1 also causes fatigue by suppressing orexin, and I did experience this.
IL-1b is also implicated in Anxiety and HPA activation [32, 33], IBS [34] (which may include excessive gas), Cognitive deficits [33], and a host of chronic diseases.
Orexin performs a number of key roles in memory acquisition and consolidation, as well as in long-term potentiation [4]. Hence, if you have elevated inflammation it will harm your cognitive performance (also by decreasing BDNF, etc). Read my article on increasing orexin.
Studies have found that higher levels of IL-1b are correlated with lower levels of testosterone [35], which helps explain why most people who I consult with that have inflammation also have low testosterone. Testosterone is a significant performance enhancer.
IL-1b can also decrease performance by decreasing the enzymes needed to make Thyroid hormones (T3) and by decreasing the receptors needed for it to function [36, 37]. And, indeed, many people with inflammation show lower levels of T3.
Cortisol also causes lower testosterone [38], but elevated IL-1 causes the release of cortisol to decrease this inflammation [1]. So it’s hard to know if IL-1 is causing lower testosterone directly or by way of increasing cortisol. It could be both.
IL-1b inhibits insulin release in response to glucose, probably as a result of increased levels of nitric oxide [39]. This leads to higher blood glucose levels, which can cause a bunch of downstream negative effects.
IL-1 decreases acetylcholine, which is a critical neurotransmitter for cognitive function and REM sleep.
Evidence suggests that IL-1 can potentiate or inhibit the effects of glutamate. IL-1b causes “synaptic hyperexcitability” and neuronal degeneration [40]. This isn’t conducive to stable thinking.
In the gut, IL-1b is a powerful inhibitor of stomach acidity. This can lead to uncontrolled H pylori infection and worsen digestion of food [41].
In general, IL-1b decreases Zinc, which is thought to be the reason that blood levels of zinc are low in rheumatoid arthritis [42].
IL-1b can contribute to diabetes by decreasing the amount of zinc your pancreas gets [43].
Some Significant Factors That Lead to Elevated IL-1b
Lectin sensitivity probably increases IL-1b in the same way that it can increase TNF [44] since these cytokines usually go together.
Fat cells produce IL-1b, so obesity will result in elevated markers of IL-1b [45]. Your weight may be causing your performance to decline.
IL-1b is increased by Sleep deprivation [46], Smoking [47], Excessive glucose/sugar [48], and Alcohol [49].
Acute exercise also causes a brief spike in IL-1b (a few hours) [50] and TNF-alpha (peaked at 14 min) [51], although this is still beneficial. I notice I get a bit fatigued after push-ups/pull-ups for a short period and this is probably why. Acute psychological stress suppresses TNF-alpha and IL-b and therefore causes wakefulness [52].
Sun/UV raises IL-1b, which suppresses orexin. This explains why we get tired if we get too much sun [53]. I still recommend time in the sun because it probably down-regulates (decreases) IL-1 production in the long term.
Moderate hypoxia (low oxygen levels) enhances IL-1b production in Macrophages [54].
Function
IL-1b has a circadian rhythm and is elevated before bed, but if you’re a night shift worker, it’s shifted to the daytime [55].
IL-1 does play a role in memory function, so you want some level of it, but as low as possible [33].
Increased free fatty acids increase IL-1Ra, leading to decreased fatigue [56]. Maybe this is why some people on a high-fat diet feel a bit better.
Excessive glucose intake causes Insulin Resistance by increasing IL-1b [48].
IL-1 plays an important role in the ovarian function and female fertility [57].
When your natural skin fungus gets out of control the body attacks it with cytokines that include IL-1b (also IL-6, TNF, IL-8), which recruits other aspects of the immune system. The resulting inflammation causes skin reddening or other symptoms.
With regard to inducing fatigue, there are two sides to the picture. IL-1 also increases wakefulness-promoting neurotransmitters to balance out the sleep-inducing effects – maintaining homeostasis. It activates Brainstem noradrenergic neurons of the locus coeruleus, dopaminergic neurons of the substantia nigra and ventral tegmental area and histaminergic neurons in the posterior hypothalamus, which are all wakefulness-promoting. However, keep in mind these are to counteract the sleep-inducing effects.
Inflammatory Diseases Associated With IL-1b
Realize that these diseases aren’t only caused by IL-1b and that not everyone with these diseases has elevated IL-1b. However, these diseases are correlated with IL-1b and the role is usually most likely causal. Also, IL-1b can be more elevated in some tissues compared to others.
- Anxiety and HPA activation [32, 33], (antagonized by MSH [32])
- IBS [34] (excessive gas), Colitis [58]
- Cognitive deficits [33]
- Heart disease [59]
- Depression [23]
- Type 2 diabetes mellitus [60]
- Insulin Resistance [48]
- Cancer in general [61] – Including Oral Cancer [62], Colon Cancer [63], Multiple Myeloma [64], Breast cancer [65]
- Acne [66] (IL-1a)
- Gout [60, 67]
- Migraines (IL-1b increases cox-2 and CGRP release)
- Psoriasis [68], Eczema [69]
- Arthritis [70] – Not as significant as the association with TNF.
- Alzheimer’s [71] (Both damaging and healing). Increases amyloid [72].
- Parkinson’s [73]
- Schizophrenia [74]
- Multiple Sclerosis [40]
- Osteoporosis (postmenopausal) [75]
- Alcohol-related liver disease [76], Chronic liver disease [77], Tinnitus [78], PCOS [79], Delirium [80]
- Diabetic neuropathy [81], Chemotherapy-induced neuropathy [82]
- Pain hypersensitivity [83]
- Behcet’s [84], Lupus -SLE [85]
- UV-induced skin damage [60], Contact allergic dermatitis [60]
- Familial Mediterranean Fever [60], Juvenile Idiopathic Arthritis [86], Endometriosis [87], Anorexia Nervosa [88] – contradictory [89].
Inhibiting Il-1b
- Cod liver/Fish oil/DHA [90]
- Jasmine Tea/Tea Polyphenols [91]
- Kombucha/Lactic acid [92]
- Black Cumin Seed Oil [93]… not bad [94]
- Cinnamon/Sodium Benzoate
- Raw honey [95]
- Stevia [96, 97]
- Goldenberries [98]
- Trehalose [99, 100]
- LLLT [101]
- Fasting [56] (Increases IL-1Ra)
Hormones
- a-MSH [102] – Also lessens the stimulatory effects of IL-1b on the HPA axis [103].
- ACTH [102]
- Testosterone [104]
- Ghrelin [105]
Supplements
- Andrographis [106] – Out of 20 plants, Andrographis inhibited IL-1b the most and was more potent than dexamethasone.
- PQQ [107]
- Fisetin [108]
- Gynostemma [109]
- Curcumin [68] – Powerful suppression in response to IMQ [110]
- Trans-Resveratrol 500mg +5g Leucine [111, 112]
- Luteolin [113]
- EGCG [114] – Powerful [115]
- Apigenin [116]
- Boswellia [117]
- Hydroxytyrosol [118] (not potent)
- Pterostilbene [119] (Strong… 30uM)
- Reishi [120] – Powerful
- L Plantarum [121] – for the gut especially.
Foods
In general, vegetables and fruit should help decrease IL-1b.
- Cyanidin-3-O-β-glucoside (C3G) – typical anthocyanin [122] – Found in many fruits.
- Ginger [106] – Has lectins, but was one of the most potent out of 20 medicinal plants [106].
- Sulforaphane/Broccoli sprouts/Cruciferous Vegetables [123].
- Anthocyanins (from red raspberries) [124].
- Oat polyphenols [125]
- Astaxanthin in fish [126].
- Betalain/Beets [127]
Other IL-1b Inhibitors
- Bile [128]
- Vitamin A/Retinol [129]
- B-glucans [130]
- MDMA (Drug) [131]
- Autophagy – The natural breaking down of what is unnecessary in the body.
- Tart Cherry Extract [132]
- Sialic Acid [133]
- Berberine [134]
- Grape Seed Extract [135]
- Chinese Skullcap/Baicalin [136, 137]
- Ashwagandha (IL-1)
- Slippery elm [138]
- Rhodiola [139]
- Silymarin [140]
- Astragalus [141]
- Rosmarinic acid [142]
- Danshen/Salvia Miltiorrhiza [143]
- Magnolol [144]
- Echinacea [145], Cichoric acid (from Echinacea) [146]
- Mannose? [147]
- Rhubarb/Emodin (found in Resveratrol pills, Rhubarb, Aloe) [148]
- Atractylodes/Atractylenolide I (IL-1)
- Zinc (if deficient) [149]
- Alfalfa [150]
- Perilla [151], Rapamycin – longevity drug [152], Electroacupuncture (IL-1) [153], Mizolastine (antihistamine) (IL-1) [154], Canakinumab (drug).
- Pathways: PPARy (IL-1a) [155], ACE inhibitors (IL-1) [156].
IL-1b Increasers
- Sleep deprivation [157]
- Smoking [47]
- Excessive glucose [48]
- Alcohol [49]
- Zinc deficiency [149]
- Aldosterone [158, 159] – From ingesting too much salt [160]
- Exercise [50, 161, 162] – But only shortly after. Increased in muscle cells in the long term.
- Melatonin [163] (IL-1)
- Vitamin C deficiency [164]
- Goji Berries [165]
- Lithium [166]
- Aloe – in cancer cells [167], Cat’s Claw [167], Grape powder – in response to LPS [168], Agmatine, Mannose-Binding Lectin [169]
- S Boulardii [170] and Bacillus Subtilis [170].
IL-1b can become elevated in response to various infections. For example, people with lingering symptoms from Lyme have elevated IL-1b [171].
Elevated IL-1 and Chronic Infection
Its possible IL-1 is activated by a chronic infection. An infection can also cause Lectin Sensitivity. Many herbs should help here, but in some instances, antibiotics are more useful.
Antibiotics like doxycycline should be explored as a last resort. While Doxycycline may not work and may have some side effects, at least it has some potential benefits. Doxycycline is a nootropic, so it increases the creation of new brain cells and reduces microglia in the hippocampus (memory center) [172] and has been found to extend worm lifespans [173]. Minocycline also increases the creation of new brain cells in adults [174] and lifespan in flies [175].
